CHAPTER 1130. HOSPICE SERVICES
GENERAL PROVISIONS Sec.
1130.1. Statutory basis.
1130.2. Policy.
1130.3. Definitions.
RECIPIENT ELIGIBILITY AND DURATION
OF COVERAGE
1130.21. Recipient eligibility requirements.
1130.22. Duration of coverage.
1130.23. Scope of benefits for General Assistance recipients.
ELECTION AND REVOCATION OF HOSPICE CARE
1130.41. Election of hospice care.
1130.42. Revocation of hospice care.
CONDITIONS OF PARTICIPATION
1130.51. Provider enrollment requirements.
1130.52. Ongoing responsibilities of hospice providers.
COVERED SERVICES
1130.61. Prerequisites for coverage.
1130.62. Covered services.
1130.63. Limitations on coverage.
PAYMENT FOR HOSPICE CARE
1130.71. General payment policy.
1130.72. Payment for physicians’ services.
1130.73. Additional payment for nursing facility residents.
UTILIZATION CONTROL
1130.81. Scope of utilization review process.
ADMINISTRATIVE SANCTIONS
1130.91. Provider misutilization.
RIGHT OF APPEAL
1130.101. Hospice right of appeal.Authority The provisions of this Chapter 1130 issued under section 443.2 of the Public Welfare Code (62 P. S. § 443.2), unless otherwise noted.
Source The provisions of this Chapter 1130 adopted June 22, 1990, effective retroactive to January 1, 1989, 20 Pa.B. 3499, unless otherwise noted.
GENERAL PROVISIONS
§ 1130.1. Statutory basis.
This chapter implements section 1905(o) of the Social Security Act (42 U.S.C.A. § 1396d(o)). Section 1905(a)(18) lists hospice care as a MA service. Section 1905(o) defines hospice care.
§ 1130.2. Policy.
The MA Program covers hospice care furnished to eligible MA recipients by hospices enrolled in the Program. Payment for hospice care is subject to this chapter, Chapters 1101 and 1150 (relating to general provisions; and MA Program payment policies) and the procedures listed in the MA Program fee schedule.
§ 1130.3. Definitions.
The following words and terms, when used in this chapter, have the following meanings, unless the context clearly indicates otherwise:
Attending physician—A physician who is:(i) A doctor of medicine or osteopathy.
(ii) Identified by the recipient, at the time he elects to receive hospice care, as having the most significant role, in the determination and delivery of medical care to the recipient.
Bereavement counseling—Guidance and spiritual support provided to the recipient’s family after the recipient’s death.
Certification period—A period of 60 consecutive days, at the beginning of which a certification of terminal illness has been filed under § 1130.22 (relating to duration of coverage).
Core services—Nursing care, medical social services, physician services and counseling services as specified in Medicare regulations at 42 CFR 418.82—418.88 (relating to core services).
Employe of the hospice—An individual performing a substantial and regular service for the hospice either for remuneration by the hospice provider or on a voluntary basis. The term includes an individual who provides some services on a voluntary basis and receives payment for other services and an individual who is appropriately trained and assigned to the hospice unit if the hospice is a subdivision of an agency or organization.
Freestanding hospice—A hospice that is not part of another type of participating provider.
Hospice—A public agency or private organization or subdivision of either of these that is primarily engaged in providing care to terminally ill individuals.
Hospice services—Services that are reasonable and necessary for the palliation or management of the recipient’s terminal illness and related conditions.
Representative—A person who, because of the recipient’s mental or physical incapacity, is authorized in accordance with State law to execute or revoke an election for hospice care or terminate curative medical care on behalf of the terminally ill recipient.
Terminally ill—A recipient who has a medical prognosis that his life expectancy is 6 months or less.
Unrelated condition—A health problem that could not reasonably be expected to be caused by the terminal illness. The term includes a dental abscess in a recipient with terminal cancer of the colon and a nonpathologic fracture or other injury sustained by a recipient with lung cancer; a pre-existing condition such as diabetes would also be considered unrelated to a terminal diagnosis such as leukemia.
Cross References This section cited in 55 Pa. Code § 1130.41 (relating to election of hospice care); and 55 Pa. Code § 1130.51 (relating to provider enrollment requirements).
RECIPIENT ELIGIBILITY AND DURATION OF COVERAGE
§ 1130.21. Recipient eligibility requirements.
To be eligible to elect hospice care under the MA Program, an individual shall:
(1) Be categorically or medically needy.
(2) Be residing at home, which includes the recipient’s home, a friend’s home, a relative’s home, a hotel, a boarding house, a personal care home, a domiciliary care facility, an intermediate care facility or a skilled nursing facility. The individual may not be residing in a hospital.
(3) Be certified as being terminally ill by a doctor of medicine or osteopathy under § 1130.22 (relating to duration of coverage).
(4) Agree to waive rights to MA Program coverage for the following services for the period during which the recipient is under the care of a designated hospice:
(i) Hospice care provided by a hospice other than the hospice designated by the recipient, unless provided under arrangements made by the designated hospice.
(ii) MA services related to the treatment of the terminal condition for which hospice care was elected or a related condition or services that are equivalent to hospice care except for:
(A) Services provided by the designated hospice.
(B) Services provided by another hospice under arrangements made by the designated hospice.
(C) Services provided by the recipient’s attending physician if that physician is not an employe of the designated hospice or receiving compensation from the hospice for those services.
(D) Medications prescribed for conditions clearly unrelated to the terminal illness.
Cross References This section cited in 55 Pa. Code § 1130.22 (relating to duration of coverage); and 55 Pa. Code § 1130.42 (relating to revocation of hospice care).
§ 1130.22. Duration of coverage.
There is no limit on the available number of days of hospice coverage for a recipient who meets the eligibility requirements of § 1130.21 (relating to recipient eligibility requirements) and who is certified as being terminally ill in accordance with the following procedures:
(1) Basic requirement. For the first 60-day period of hospice coverage, the hospice obtains, within 2 calendar days after hospice care is initiated, a completed certification of terminal illness form signed by:
(i) The medical director of the hospice or the physician member of the hospice interdisciplinary group.
(ii) The recipient’s attending physician if the recipient has an attending physician.
(2) Exception. For the first 60-day period of hospice coverage, if the hospice cannot obtain a completed and signed certification of terminal illness form within 2 calendar days after hospice care is initiated, it shall obtain oral certification within 2 calendar days and a completed and signed certification form within 8 calendar days after hospice care is initiated.
(i) Oral certification. Hospice staff persons shall make an appropriate entry in the recipient’s medical records as soon as they receive an oral certification.
(ii) Written certification. The hospice shall obtain within 8 calendar days after hospice care begins, a completed certification of terminal illness form signed by the following:
(A) The medical director of the hospice or the physician member of the hospice interdisciplinary group.
(B) The recipient’s attending physician, if the recipient has an attending physician.
(3) Subsequent periods. For each subsequent 60-day period, the hospice obtains, within 2 calendar days after the beginning of that period, a certification of terminal illness form completed and signed by the medical director of the hospice or the physician member of the hospice’s interdisciplinary group.
(4) Certification form. The certification of terminal illness shall be carried out using the Department’s certification of terminal illness form specified in Appendix A.
(5) Record retention. The hospice shall retain the certification statements described in this section for 4 years.
Source The provisions of this § 1130.22 amended January 24, 1992, effective August 17, 1991, 22 Pa.B. 361. Immediately preceding text appears at serial pages (150020) to (150021).
Cross References This section cited in 55 Pa. Code § 1130.3 (relating to definitions); 55 Pa. Code § 1130.21 (relating to recipient eligibility requirements); 55 Pa. Code § 1130.42 (relating to revocation of hospice care); and 55 Pa. Code § 1130.61 (relating to prerequisites for coverage).
§ 1130.23. Scope of benefits for General Assistance recipients.
General Assistance recipients, age 21 to 65, whose MA benefits are funded solely by State funds, are eligible for medically necessary basic health care benefits as defined in Chapter 1101 (relating to general provisions). See § 1101.31(e) (relating to scope).
Source The provisions of this § 1130.23 adopted December 11, 1992, effective January 1, 1993, 22 Pa.B. 5995.
ELECTION AND REVOCATION OF HOSPICE CARE
§ 1130.41. Election of hospice care.
(a) Election statement. If a recipient who meets the eligibility requirements for hospice care elects to receive that care, the recipient or the recipient’s representative shall file, with a particular hospice, the election statement specified in Appendix B.
(b) Effective date of election. An election date may not be a date that is earlier than the date the election is made.
(c) Change of designated hospice. The recipient or the recipient’s representative may change the designation of the hospice from which the recipient wishes to receive care once in each certification period as defined in § 1130.3 (relating to definitions). To change hospices, the recipient or the recipient’s representative shall file with the hospice from which care has been received and with the newly designated hospice, the change of hospice statement specified in Appendix C.
Cross References This section cited in 55 Pa. Code § 1130.61 (relating to prerequisites for coverage).
§ 1130.42. Revocation of hospice care.
(a) Right to revoke. The recipient or the recipient’s representative may revoke the recipient’s election of hospice care at any time. To revoke the election of hospice care, the recipient, or the recipient’s representative shall file with the hospice the revocation statement specified in Appendix D.
(b) Effect of revocation. A recipient who revokes the election of hospice care:
(1) Is no longer covered under the MA Program for hospice care.
(2) Resume full MA Program coverage as applicable to the recipient’s category of assistance at the time of revocation, including those services waived under § 1130.21(a)(4) (relating to recipient eligibility requirements).
(3) May elect, at any time, to resume hospice coverage under § 1130.22 (relating to duration of coverage).
(c) Certification. If a recipient revokes hospice care and reelects hospice care with the same hospice during the same certification period, a new certification of terminal illness is not required until the beginning of the subsequent certification period.
CONDITIONS OF PARTICIPATION
§ 1130.51. Provider enrollment requirements.
To qualify for enrollment as a provider of hospice services under the MA Program, a hospice shall:
(1) Meet the definition of a hospice in § 1130.3 (relating to definitions).
(2) Be Medicare certified.
(3) Comply with the prerequisites for participation established in § § 1101.11, 1101.42 and 1101.43(b)(1) and (5) (relating to general provisions; prerequisites for participation; and enrollment and ownership reporting requirements).
§ 1130.52. Ongoing responsibilities of hospice providers.
(a) To retain the right to participate in the MA Program, a provider of hospice services shall:
(1) Be Medicare certified and continue to meet the Medicare conditions for participation as a hospice as set forth at 42 CFR Part 418, Subpart C (relating to conditions of participation).
(2) Fulfill the applicable requirements of § § 1101.42, 1101.43(b)(1) and (5) and 1101.51 (relating to prerequisites for participation; enrollment and ownership reporting requirements; and ongoing responsibilities of providers).
(3) Fully inform each recipient or representative, in writing prior to admission to the hospice, regarding the following:
(i) Conditions the hospice imposes.
(ii) What services the hospice provides.
(iii) The names of other facilities such as hospitals and nursing facilities with which the hospice has agreements for general inpatient or respite care.
(iv) The recipient’s rights under the MA Program with respect to changing the designated hospice, revoking hospice care and receiving care from a physician of the patient’s choice.
(v) The fact that the recipient may be notified by the CAO that he is required to pay a specific amount towards hospice care, with respect to a recipient residing in a nursing facility.
(4) Ensure that enrollment of MA recipients in a hospice is without regard to age, race, creed, sex, physical or mental handicap, national origin, marital status or sexual preference.
(5) Not contract or otherwise arrange for hospice service to be provided either directly or indirectly to a MA recipient by a provider who has been suspended or terminated from participation in the MA Program.
(b) The hospice organization elected by the recipient is considered by the Department to be the responsible provider of hospice services and will be held ultimately responsible for the quality of services rendered.
(c) The hospice is responsible for notifying, in writing, the CAO, within 7 calendar days, when a MA recipient elects hospice care, revokes hospice care, changes to a different hospice or dies.
COVERED SERVICES
§ 1130.61. Prerequisites for coverage.
To be covered, hospice services shall meet the following requirements:
(1) The services shall be reasonable and necessary for the palliation or management of the symptoms of the terminal illness as well as related conditions.
(2) The recipient shall have elected hospice care under § 1130.41 (relating to election of hospice care).
(3) A plan of care shall be established in accordance with Medicare regulations at 42 CFR 418.58 (relating to condition of participation—plan of care) before the services are provided.
(4) The services shall be consistent with the plan of care.
(5) A certification that the individual is terminally ill shall be completed under § 1130.22 (relating to duration of coverage).
§ 1130.62. Covered services.
The following services are covered hospice services when provided in accordance with the Medicare regulations at 42 CFR 418.202 (relating to covered services):
(1) Nursing care.
(2) Medical social services.
(3) Physicians’ services.
(4) Counseling services.
(5) Short-term inpatient care.
(6) Medical supplies and appliances.
(7) Drugs that are used primarily for the relief of pain and symptom control related to the terminal illness.
(8) Home health aide services.
(9) Physical therapy, occupational therapy and speech-language pathology services.
§ 1130.63. Limitations on coverage.
(a) Nursing care may be covered on a continuous basis for as much as 24 hours a day during periods of crisis as necessary to maintain the recipient at home. Homemaker or home health aide services, or both, may be covered on a 24-hour continuous basis during periods of crisis, but care during these periods shall be predominantly nursing care as described by Medicare regulations at 42 CFR 418.202(a) (relating to covered services).
(b) Respite care may not exceed a total of 5 days in a 60-day certification period.
(c) Bereavement counseling is a required hospice service but it is not reimbursable.
(d) General inpatient care shall be provided in a general hospital, skilled nursing facility or a freestanding hospice participating in the MA Program.
(e) An intermediate care facility may provide only respite care services to the hospice. Eligible MA recipients residing in an intermediate care facility may elect to receive care from a participating hospice.
(f) Hospice providers may arrange for respite care services only in those intermediate care facilities that meet the Medicare regulations at 42 CFR 418.100(a) and (f) (relating to condition of participation for freestanding hospices providing inpatient care directly) regarding 24-hour nursing services and patient areas.
PAYMENT FOR HOSPICE CARE
§ 1130.71. General payment policy.
(a) Payment is made to a participating hospice in accordance with the coverage and payment rates established by Medicare regulations at 42 CFR 418.302 (relating to payment procedures for hospice care). Exceptions are as follows:
(1) A recipient with a confirmed diagnosis of acquired immune deficiency syndrome (AIDS) will not be counted when calculating the hospice inpatient care limit established by Medicare regulations at 42 CFR 418.302(f).
(2) A hospice provider will not be subject to the annual cap on overall payments as described by Medicare regulations at 42 CFR 418.309 (relating to hospice cap amount).
(b) Payment is made to the hospice for each day during which the recipient is eligible and under the care of the hospice, regardless of the amount of services furnished on a given day.
(1) If admission and discharge, revocation or death occur on the same day, the day will be considered a hospice care day and the hospice will be paid at the rate commensurate with the level of care provided.
(2) If the level of care changes, payment will be made for the new level of care beginning with the day it commences.
(3) If a change of hospice occurs, payment will not be made to the discharging hospice for the day of discharge. Payment will be made to the newly elected hospice.
(4) If the recipient is discharged from an inpatient unit, the routine home care rate will be paid unless the recipient dies as an inpatient. If the recipient is discharged deceased, the general inpatient or respite care rate will be paid for the discharge date.
(c) Payment is not made for days not covered by a valid certification of terminal illness.
(d) Payment for inpatient respite care is limited to no more than a total of 5 days in a 60-day certification period. Payment for inpatient respite care days in excess of the limit will be made at the routine home care rate.
(e) Payment is not made for general inpatient care if the Department determines that a lesser level of care was actually provided.
(f) No MA payments will be made directly to a nursing facility for services provided to a recipient who is under the care of a hospice.
(g) Ambulance transportation related to management of the recipient’s terminal illness is included in the daily rates. A separate payment will not be made to the hospice provider or to an ambulance provider for this service.
(h) The Department will reduce its payment for hospice care by the amount of income available from the recipient towards the hospice care rate established by the Department.
§ 1130.72. Payment for physicians’ services.
(a) The following services performed by hospice physicians are included in the level of care rates paid for a day of hospice care:
(1) General supervisory services of the medical director.
(2) Participation in the establishment of plans of care, supervision of care and services, periodic review and updating of plans of care and establishment of governing policies by the physician member of the interdisciplinary group.
(b) For physicians’ services not described in subsection (a), payment will be made to the hospice in accordance with the MA Program Fee Schedule.
(c) Services of the recipient’s attending physician are paid directly to that physician in accordance with the MA Program Fee Schedule if the physician is not an employe of the hospice or providing services under arrangement with the hospice.
(d) Services provided to treat a condition that is clearly unrelated to the terminal illness are not considered hospice services. The services are compensable to the appropriate provider in accordance with the applicable MA Program regulations.
§ 1130.73. Additional payment for nursing facility residents.
(a) An additional payment is made to a hospice for hospice care furnished to a MA recipient who is a resident of a skilled or intermediate care facility participating in the MA Program. The additional payment will take into account the cost of room and board. Room and board rates will be calculated as follows:
(1) Room and board cost data will be retrieved from the most recently audited cost reports of participating skilled nursing facilities.
(2) Appropriate inflation factors will be applied to each facility’s room and board cost as needed to bring it forward to Fiscal Year 1989-90.
(3) The costs will be grouped into Metropolitan Statistical Areas (MSAs) according to the location of the nursing facility.
(4) An average room and board per diem will be calculated for each group.
(5) A wage index appropriate to each MSA will be applied to the average room and board per diem to account for area differences in wages.
UTILIZATION CONTROL
§ 1130.81. Scope of utilization review process.
Hospice services provided to MA recipients are subject to the utilization review procedures established under Chapter 1101 (relating to general provisions).
ADMINISTRATIVE SANCTIONS
§ 1130.91. Provider misutilization.
If the Department determines that a provider billed for services inconsistent with this chapter and Chapter 1101 (relating to general provisions), provided incorrect information on the billing invoice regarding a recipient’s diagnosis or the services provided during the period the recipient was under the care of the hospice or otherwise violated the standards set forth in the provider agreement, the provider is subject to the sanctions described in Chapter 1101.
RIGHT OF APPEAL
§ 1130.101. Hospice right of appeal.
(a) The hospice’s right of appeal is set forth at Chapter 1101 (relating to general provisions).
(b) Hospice providers and hospice physicians do not have the right to separate appeals on the same case.
(c) For cases undergoing the appeal process, payment including adjustments will be withheld until the case is adjudicated.
APPENDIX A

Cross References This appendix cited in 55 Pa. Code § 1130.22 (relating to duration of coverage).
APPENDIX B


Cross References This appendix cited in 55 Pa. Code § 1130.41 (relating to election of hospice care).
APPENDIX C

Cross References This appendix cited in 55 Pa. Code § 1130.41 (relating to election of hospice care).
APPENDIX D
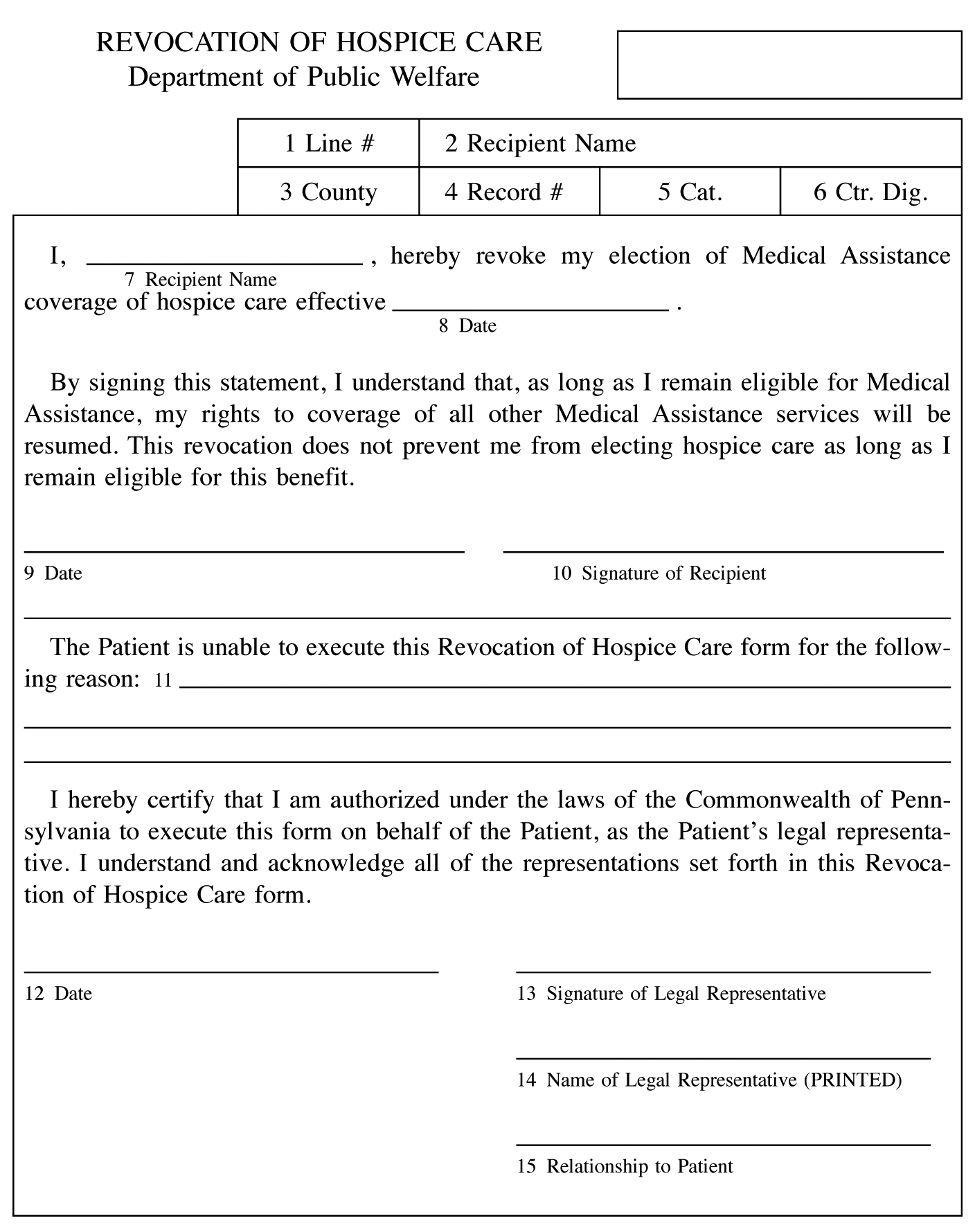
Cross References This appendix cited in 55 Pa. Code § 1130.42 (relating to revocation of hospice care).
No part of the information on this site may be reproduced for profit or sold for profit.
This material has been drawn directly from the official Pennsylvania Code full text database. Due to the limitations of HTML or differences in display capabilities of different browsers, this version may differ slightly from the official printed version.